Contents
- 1 Total Knee Replacement
- 1.0.1 Who is a candidate for total knee replacement?
- 1.0.2 What are the risks of total knee replacement?
- 1.0.3 What is the pre-operative assessment for total knee replacement?
- 1.0.4 What is recovery from total knee replacement?
- 1.0.5 What is the rehabilitation for total knee replacement?
- 1.0.6 Subscribe to MedicineNet’s Arthritis Newsletter
Total Knee Replacement
A total knee replacement is a surgical procedure where the diseased knee joint is replaced with artificial material. The knee is a hinge joint that provides motion at the point where the thigh meets the lower leg. The thighbone (or femur) abuts the large bone of the lower leg (tibia) at the knee joint.
During a total knee replacement, the end of the femur bone is removed and replaced with a metal shell. The end of the lower leg bone (tibia) is also removed and replaced with a channeled plastic piece with a metal stem. Depending on the condition of the kneecap portion of the knee joint, a plastic "button" may also be added under the kneecap surface. The artificial components of a total knee replacement are referred to as the prosthesis.
The posterior cruciate ligament normally stabilizes each side of the knee joint so that the lower leg cannot slide backward in relation to the thighbone. In total knee replacement surgery, this ligament is either retained, sacrificed, or substituted by a polyethylene post. Each design of total knee replacement has its own particular benefits and risks.
Who is a candidate for total knee replacement?
Total knee replacement surgery is considered for patients with knee joints damaged by progressive arthritis, trauma, or other rare destructive joint diseases. The most common reason for knee replacement in the United States is severe osteoarthritis.
Regardless of the cause of joint damage, the resulting increasing pain, stiffness, and decreasing daily function lead patients to consider total knee replacement. Decisions about knee replacement surgery are not easy. Patients should understand the risks and benefits before making these decisions.
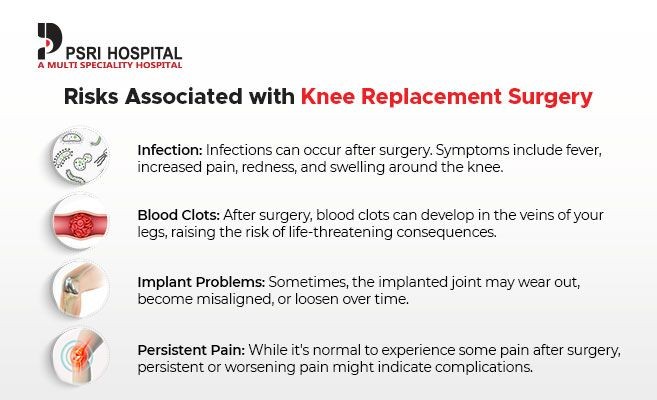
What are the risks of total knee replacement?
Risks of total knee replacement include blood clots in the legs that can travel to the lungs (pulmonary embolism).
- Pulmonary embolism can cause shortness of breath, chest pain, and shock.
- Other risks include urinary tract infection, nausea, vomiting, chronic knee pain and stiffness, bleeding into the knee joint, nerve damage, blood vessel injury, infection of the knee requiring reoperation, potential heart, lung, kidney, and liver damage.
What is the pre-operative assessment for total knee replacement?
Before surgery, the adjacent joints to the diseased knee (hip and ankle) are evaluated. This is important to ensure optimal outcome and recovery from the surgery. Replacing a knee joint adjacent to a severely damaged joint may not yield a significant improvement in function.
- All medications that the patient is taking are reviewed. Blood-thinning medications such as warfarin (Coumadin) and anti-inflammatory medications such as aspirin may need adjustment or to be discontinued prior to knee replacement surgery.
- Routine blood tests of liver and kidney function and urine tests are evaluated for signs of abnormality.
- Chest X-ray and EKG are performed to exclude significant heart and lung disease that may prevent surgery or anesthesia.
- A good long-term outcome of knee replacement is less likely if the patient’s weight exceeds 200 pounds.
Another risk is encountered in younger patients who may tend to be more active, thereby adding trauma to the replaced joint.
What is recovery from total knee replacement?
A total knee replacement generally requires between one and a half to three hours of operative time. Post-surgery, patients are taken to a recovery room, where vital organs are frequently monitored. When stabilized, patients are returned to their hospital room.
- Passage of urine can be difficult in the immediate postoperative period, and this condition can be aggravated by pain medications. A catheter inserted into the urethra (a Foley catheter) allows free passage of urine until the patient becomes more mobile.
- Physical therapy is an important part of rehabilitation and requires full participation by the patient for optimal outcomes. Patients can begin physical therapy 48 hours after surgery.
- Some degree of pain, discomfort, and stiffness can be expected during the early days of physical therapy.
- Knee immobilizers are used to stabilize the knee while undergoing physical therapy, walking, and sleeping. They may be removed under the guidance of the physical therapist for various portions of physical therapy.
- A continuous passive motion (CPM) machine can help speed recovery. The machine constantly moves the knee through various degrees of range of motion for hours while the patient relaxes, improving circulation and minimizing the risk of scarring and contracture of the tissues around the knee.
- Patients will start walking using a walker and crutches. Eventually, patients will learn to walk up and downstairs and grades.
- Several home exercises are given to strengthen the thigh and calf muscles.
What is the rehabilitation for total knee replacement?
For an optimal outcome after total knee replacement surgery, patients should participate in an outpatient physical therapy program along with home exercises. The muscles around the replaced joint should be exercised to prevent scarring and maintain muscle strength for joint stability. These exercises can reduce recovery time and lead to optimal strength and stability.
The wound will be monitored for healing and patients should watch for signs of infection. It is important to report any injury to the joint to the doctor immediately.
Future activities should avoid injuring the replaced joint. Sports that involve running or contact should be avoided, in favor of leisure sports such as golf and swimming. Swimming is the ideal form of exercise since it improves muscle strength and endurance without exerting any pressure or stress on the replaced joint.
Patients with joint replacements should inform their doctors and dentists about their artificial joint as it is at risk for infection from invasive procedures or infections in the body. Antibiotics may be prescribed before, during, and after any elective procedures to prevent infection of the replaced joint.
Though infrequent, patients with total knee replacements may require a second operation years later due to complications. Reoperations carry higher risks of complications and are generally not as successful as the original operation. Future advancements will improve patient outcomes and reduce complications.
Subscribe to MedicineNet’s Arthritis Newsletter
By clicking "Submit," I agree to the MedicineNet Terms and Conditions and Privacy Policy. I also agree to receive emails from MedicineNet and understand that I may opt out of MedicineNet subscriptions at any time.
Klippel, John H., eds., et al. Primer on the Rheumatic Diseases. New York: Springer and Arthritis Foundation.