Juvenile Rheumatoid Arthritis (JRA)
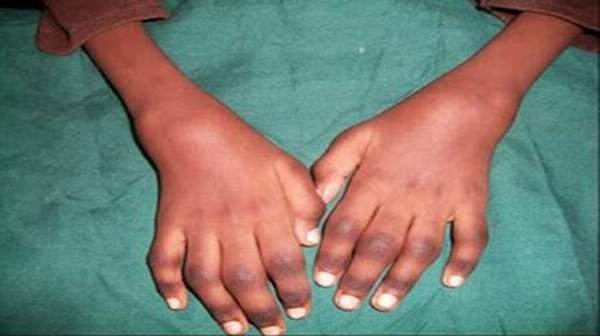
Juvenile rheumatoid arthritis (JRA) is a term used to categorize several forms of chronic arthritis in children. These conditions share common historical and clinical characteristics. Inflammation in one or more joints is evident with symptoms like swollen joints, limited range of motion, joint tenderness, and increased warmth. These symptoms must be present for at least six weeks and affect children younger than 16 years of age.
JRA is the most common chronic rheumatologic disease in childhood, and its causes are not well understood. Genetic and environmental factors are believed to contribute to the development of signs and symptoms. Knowledgeable specialists, such as pediatric rheumatologists, can help prevent complications such as leg-length discrepancy, joint contractures, and eye inflammation (iritis) that can lead to blindness.
Previously known as JRA in the US and JCA in Europe, JIA is now the accepted term to distinguish it from rheumatoid arthritis. This new classification has helped improve communication among researchers studying the causes, clinical manifestations, and therapy of JIA. Six subtypes of JIA have been identified.
JRA is considered a diagnosis of exclusion and can only be confidently made when the patient’s history, physical exam, and laboratory findings align with the literature provided by the International League of Associations for Rheumatology. Other conditions must be ruled out, including infection, malignancy, trauma, reactive arthritis, immunodeficiency, and other connective tissue/rheumatologic diseases like systemic lupus erythematosus.
Causes and Risk Factors of Juvenile Rheumatoid Arthritis
While the specific causes of JRA are unknown, genetic and environmental factors are thought to play a role. Studies have shown that if one identical twin develops the disease, there is a 25%-40% chance of the other twin developing it as well. Nonidentical siblings also have a significantly increased risk, up to 15 to 30 times higher than the general pediatric population.
JRA’s biological and clinical manifestations indicate an immune system misdirection. Both the cell-based and humeral-based arms of the immune system react against the body’s own structures, such as joints, muscles, and eye tissues. Researchers are conducting ongoing research to better understand this auto-inflammatory process and develop more effective treatments and eventually a cure for JRA.
The Six Types of Juvenile Rheumatoid Arthritis (JRA)
JRA can be classified into six broad categories:
- Systemic onset JRA
- Oligoarticular JRA (divided into two subgroups)
- Polyarticular JRA (divided into two subgroups)
- Psoriatic arthritis
- Enthesitis-related arthritis
- Undifferentiated arthritis
Each of these types has distinct clinical presentations, symptoms, laboratory implications, potential complications, and treatment options. Morning stiffness that improves with movement is a common characteristic among all six types. Spontaneous patterns of symptom worsening and lessening, independent of therapy, are also typical.
Accurate diagnosis and prognosis for each category require specific criteria, which are detailed below.
Systemic Onset JRA
Systemic onset JRA is characterized by arthritis in one or more joints accompanied by at least two weeks of daily spiking fevers. The fever often exceeds 102 F (39 C) and spikes once or twice a day. Other symptoms may include a salmon-colored rash, swollen lymph nodes, liver, spleen, and inflammation of organs like the lungs and pericardium. Children appear moderately sick during febrile episodes but greatly improve when the fever resolves.
- About 10%-15% of children with JRA experience systemic onset JRA.
- There is no gender preference, and symptoms typically start between the ages of 3 and 5.
- No specific laboratory test exists, but anemia, elevated white blood cell and platelet counts, and general markers of inflammation are usually present.
- Complications may include slower growth, weakened bones, and abnormalities in liver and lung function, in addition to therapy-related consequences.
Oligoarticular JRA
Oligoarticular JRA is characterized by arthritis affecting four or fewer joints in the first six months of the disease. It accounts for approximately 50% of all cases of pediatric chronic arthritis and can be divided into two groups.
- One group continues to have four or fewer joints involved throughout the course of the disease.
- The other group develops greater than four-joint involvement after the first six months.
Oligoarticular JRA usually appears between the ages of 2 and 4, with a 3:1 female gender bias. The knee is the most commonly affected joint, accounting for about 90% of cases. Symptoms include joint pain, tenderness, and morning stiffness. The primary complication of oligoarticular JRA is inflammation of the iris, which occurs in approximately 15%-20% of cases and may be asymptomatic. Complications of iritis include cataracts, glaucoma, and vision loss.
Early diagnosis is crucial, and regular ophthalmologic evaluations every three to four months are necessary. Trauma, infection, malignancy, and arthritis following an infection should be ruled out before diagnosing oligoarticular JRA.
Polyarticular JRA
Polyarticular JRA is characterized by arthritis affecting five or more joints during the first six months of the disease. Two subgroups of this form exist based on various laboratory studies.
- The "RF positive" subgroup affects 5%-10% of JRA patients and predominantly occurs in late childhood through adolescence. Small joints, like the hands and feet, are commonly involved, and the course tends to be more aggressive. The "RF negative" subgroup has a milder course and better outcome.
- Complications may include fatigue, anemia, suboptimal growth, and iritis, although to a lesser degree than in oligoarticular JRA. Infectious, malignant, and collagen vascular diseases like systemic lupus erythematosus must be ruled out before diagnosing polyarticular JRA.
Psoriatic Arthritis (PsA)
Psoriatic arthritis is diagnosed when both large and small joint arthritis and a characteristic rash (psoriasis) are present. If the rash is absent, two of the following must exist: a family history of psoriasis, diffuse swelling of the fingers, and pitting of the nails. Children with psoriatic arthritis should undergo ophthalmologic evaluations every six months.
Enthesitis-Related Arthritis (ERA)
Enthesitis-related arthritis primarily affects males over the age of 8 and is characterized by inflammation at the site where tendons attach to the bone. It often involves the lower back, sacroiliac joints, and joints of the legs, ankles, and feet. Individuals with a specific genetic marker (HLA-B27) may also develop iritis, inflammatory bowel disease, psoriasis, or ankylosing spondylitis. The male-to-female ratio is 7:1.
Undifferentiated Arthritis
Undifferentiated arthritis is diagnosed when a patient does not fit clearly into any of the above subtypes of JRA or has symptoms that overlap multiple subtypes. Accurate prognosis and treatment planning are challenging due to the diverse nature of this patient population and the absence of classical history and findings from exams and laboratory studies.
Drugs That Slow
RA’s Progress
Drugs That Slow
RA’s Progress