Contents
Is Lymphangioleiomyomatosis a Fatal Disease?
Lymphangioleiomyomatosis (LAM) may shorten life expectancy; however, people with LAM are living longer than before, according to recent data. LAM can cause loss of lung function, potentially requiring a lung transplant.
- The 10-year survival rate for LAM patients ranges from 80 to 90 percent.
- The average survival time from symptom onset is about 30 years.
What is Lymphangioleiomyomatosis?
Lymphangioleiomyomatosis, also known as perivascular epithelioid cell tumor (PEComatous tumors), is a type of mesenchymal tumor that can occur in the lung, kidneys, and axial lymphatics. LAM most commonly affects women of childbearing age.
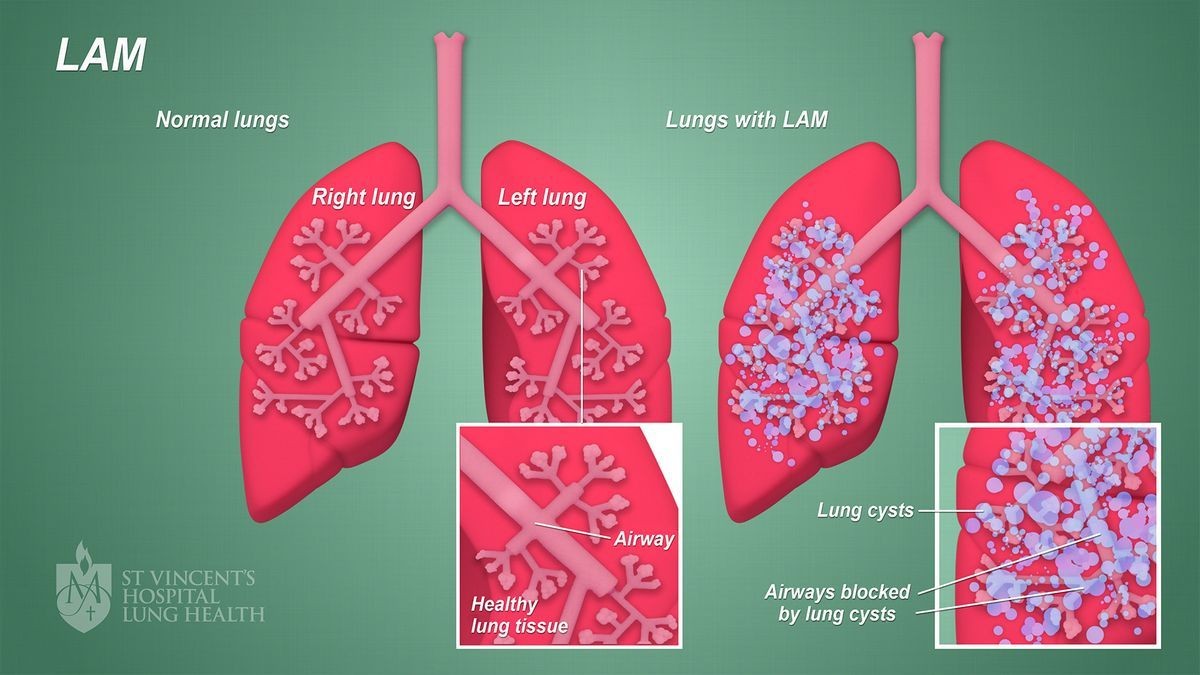
LAM is caused by mutations in the TSC2 or TSC1 genes. LAM cells grow uncontrollably in the kidneys, lymph nodes, and lungs, eroding healthy lung tissue and forming fluid-filled cysts. This can hinder oxygen supply to the body.
There are two types of LAM:
- Sporadic LAM: It occurs spontaneously and is not hereditary.
- Tuberous sclerosis complex (TSC) LAM: It is associated with TSC, an inheritable genetic condition.
What causes Lymphangioleiomyomatosis?
Lymphangioleiomyomatosis (LAM) is associated with a rare genetic disorder known as tuberous sclerosis complex. Both types of LAM are caused by mutations in the TSC1 or TSC2 genes.
In LAM, abnormal LAM cells travel through lymphatic and blood vessels and gather in the lungs, forming cysts and causing lung damage.
- In sporadic LAM, mutations are somatic and occur in peripheral tissues after conception. They are not inherited.
- In TSC LAM, mutations can be sporadic or inherited in an autosomal dominant pattern. Most cases are caused by new gene mutations and lack a family history of the illness.
What are the symptoms of Lymphangioleiomyomatosis?
Signs of Lymphangioleiomyomatosis usually appear between the ages of 20 and 40. TSC LAM often has milder symptoms than sporadic LAM, and pulmonary symptoms are not common. Untreated LAM can cause serious health problems.
Symptoms of LAM may include:
- Shortness of breath
- Cough
- Chest pain
- Fatigue
- Wheezing
- Breathlessness during physical exertion
- Hemoptysis (coughing up blood)
- Coughing up viscous white sputum
- Progressive worsening of symptoms
- Enlarged lymph nodes
- Abdominal cysts or tissue masses
Pneumothorax, the most common manifestation of LAM, occurs when a lung "pops" and air accumulates around it, causing the lung to collapse. LAM patients may also develop chyle buildup, a milky fluid surrounding the lungs.
How is Lymphangioleiomyomatosis diagnosed?
The diagnosis of Lymphangioleiomyomatosis (LAM) may involve a thorough clinical examination, including patient history and specialized tests:
- HRCT (high-resolution CT): An HRCT scan can diagnose LAM by revealing characteristic thin-walled cysts in the lungs. It can also detect angiomyolipomas or lymphangioleiomyomas in the abdomen. Chest X-rays are ineffective for diagnosing early-stage LAM.
- Blood tests: Up to 60 percent of LAM patients have increased VEGF-D levels. High VEGF-D levels, combined with distinctive CT scan results, aid in diagnosing LAM without the need for a lung biopsy.
- Lung function tests: These help establish a baseline for lung function and assist in long-term monitoring.
According to the American Thoracic Society/Japanese Respiratory Society guidelines 2017, LAM can be clinically diagnosed based on a standard lung CT and the presence of TSC, renal angiomatoma, cystic lymphangioleiomyoma, or a chylothorax/chyloperitoneum.
If TSC is not diagnosed, the guidelines recommend testing for VEGF-D before lung biopsy. Serum VEGF-D levels indicate disease severity, progression, and response to mTOR inhibitors. The diagnostic level is 800 pg/mL.
How to treat Lymphangioleiomyomatosis
Although there is no known cure for LAM, medications can manage symptoms and delay consequences. Oxygen therapy or a lung transplant may also be options.
Medications
- mTOR inhibitor therapy: Long-term use of an mTOR inhibitor helps patients with abnormal lung function and signs of deterioration. Sirolimus and everolimus are effective inhibitors that can improve lung function and quality of life in LAM patients.
- Supportive measures
- Oxygen therapy: May be necessary to maintain oxygen saturation and alleviate symptoms.
- Bronchodilators: May benefit LAM patients with a bronchodilator-responsive component.
Lung transplantation
Lung transplant assessment may be necessary for patients with severe lung function impairment or significant impact on quality of life. Both single and bilateral lung transplants are effective options for LAM patients.