Contents
Shin Splints
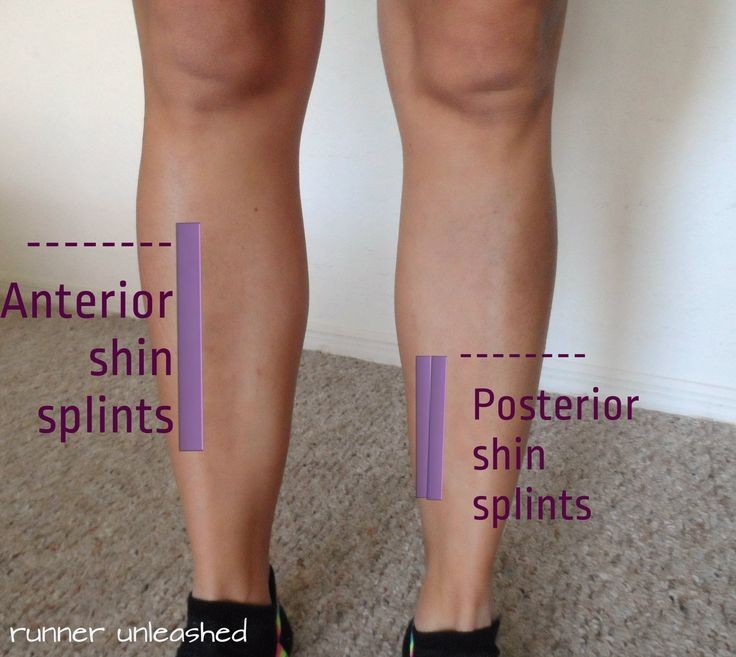
Shin splints are injuries to the front of the outer leg caused by overuse and typically happen to runners or aggressive walkers. Shin splint pain can prevent you from working out. Rest is usually the best treatment for shin splints, and you can also ice the injury and take over-the-counter (OTC) pain medicine to relieve pain.
- Shin splints are "overuse injuries" to the legs.
- The pain is located on the outer edge of the mid-region of the leg next to the shinbone (tibia). It can halt workouts.
- The diagnosis requires a focused examination.
- "Relative rest" can restore a pain-free level of activity and a return to competition.
- The relative rest approach includes changing the workout, icing the injury, resting, taking anti-inflammatory medications, stretching exercises, possibly changing footwear, and gradually increasing running activities.
- Proper footwear can help prevent shin splints.
- The outlook is excellent for full recovery, but physical therapy treatment may be necessary.
Causes of Shin Splints
- A sudden increase in distance or intensity of a workout is a primary cause of shin splints. This increase in muscle work can lead to inflammation of the lower leg muscles, especially those used in lifting the foot (the motion during which the foot pivots toward the tibia).
- A tight Achilles tendon or weak ankle muscles are also often involved in developing shin splints.
- Overdoing workouts or training too hard or too fast without gradually increasing intensity is the most common cause of shin splints.
- Inadequate support from workout shoes can also cause shin splints.
- Running or walking on a different surface than usual can trigger shin splints.
- Risk factors for shin splints include running and over-training on hills, using inadequate footwear for athletic activity, and poor biomechanics of the legs and feet.
Symptoms of Shin Splints
- Shin splints cause pain in the front of the outer leg below the knee. The pain is located on the outer edge of the mid-region of the leg next to the shinbone (tibia), usually in a 4-6 inch (10-15 cm) area.
- Pain is often felt in the early part of the workout, subsides, and then returns near the end of the training session.
- Shin splint discomfort is initially described as dull but can become extreme over time and force the athlete to stop workouts.
Diagnosis of Shin Splints
- Shin splints are usually diagnosed during a physical examination, which includes a review of the patient’s history and tenderness examination of the shins and legs.
- Specialized (and costly) tests, such as bone scans, are generally unnecessary unless the diagnosis is unclear.
- Radiology tests like X-rays, bone scans, or MRI scans can help detect stress fractures of the tibia bone.
Treatment for Shin Splints
Previously, two different treatment management strategies were used: total rest or a "run through it" approach.
- Total rest was often unacceptable to athletes.
- The "run-through" approach worsened injuries and symptoms.
Currently, a multifaceted approach of relative rest is successfully used to restore athletes to a pain-free level of competition.
Most common stretches to relieve shin splint pain:
- Foam Rolling: Kneel on the roller and gently roll down the front of the shin, repeating from the lower knee to the ankle. This should be done one to three times per week.
- Shin Stretch: Sit on feet with legs flat against the floor, slowly lean back to increase the stretch with arm support.
- Toe Pull Back: Sit with legs straight out in front and use a slow controlled motion to pull the toes back towards the torso.
- Toe Raise: Balance with heels on the edge of a step, then pull the toes upwards and in towards the shins.
- Heel Walking: Balance on the heels barefoot and walk in circles or figure eights for a set period of time.
Multifaceted Relative Rest Approach to Shin Splints
The following steps are part of the multifaceted approach:
- Use workouts like stationary bicycling or pool running to maintain cardiovascular fitness.
- Apply ice packs to reduce inflammation.
- Take anti-inflammatory medications like ibuprofen (Advil/Motrin) or naproxen (Aleve/Naprosyn).
- Wrap a 4-inch wide Ace bandage around the region or wear a Neoprene calf sleeve to reduce discomfort.
- Perform calf and anterior leg stretching and strengthening exercises to address biomechanical problems and reduce pain.
- Select the correct running shoe based on foot type, and consider using shoe inserts if necessary.
- Do stretching and strengthening exercises twice a day.
- Resume running only when symptoms have generally resolved (usually about two weeks) and with restrictions:
- A level and soft terrain is best.
- Distance is limited to 50% of the pre-injury tolerance.
- Intensity (pace) is cut by one-half.
- Over a three- to six-week period, gradually increase distance.
- Only then attempt a gradual increase in pace.
Prognosis for Shin Splints
- The extent of injury prior to rehabilitation plays a significant role in determining the recovery time.
- The outlook is excellent for full recovery, but physical therapy treatment may be necessary.
Preventing Shin Splints
Prevention tips for shin splints:
- Gradually increase exercise activities to prevent shin splints as an overuse injury.
- Use footwear that provides proper support.
- Cross-train in low-impact sports like swimming or cycling to balance out the workout.
- Incorporate strength training to develop muscles that can prevent shin splints.
- Avoid overdoing it and listen to your body to avoid further injury.
- People with poor foot mechanics or weak muscles may need physiotherapy or custom orthotics to prevent shin splints.
Firestein, G.S., et al. Kelley’s Textbook of Rheumatology, 9th Ed. Philadelphia, Pa: Saunders Elsevier, 2012.
Koopman, William, et al., eds. Clinical Primer of Rheumatology. Philadelphia: Lippincott Williams & Wilkins, 2003.