Contents
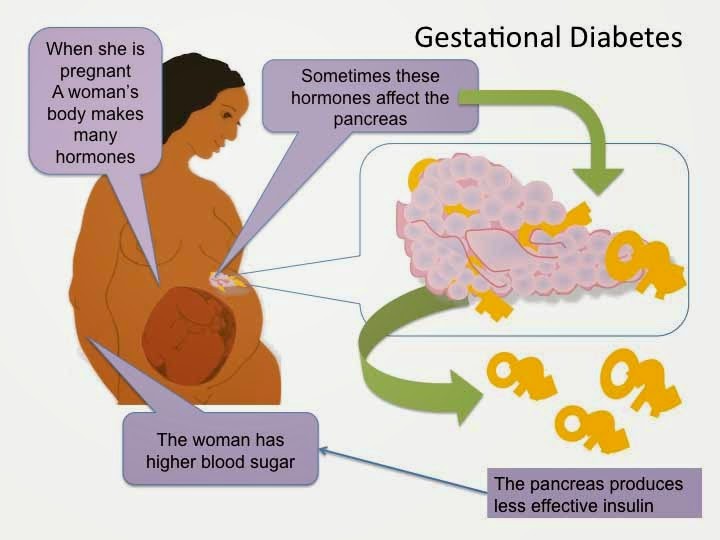
Gestational Diabetes
Gestational diabetes is diabetes that develops during pregnancy, affecting approximately 4% of all pregnancies. It is usually diagnosed in the later stages of pregnancy and often occurs in women with no prior history of diabetes.
Causes
Gestational diabetes arises due to changes that occur in the body during pregnancy, which can make some women resistant to insulin. Insulin is a hormone that allows the body to metabolize glucose for energy. When levels of insulin are low or the body cannot effectively use insulin (insulin resistance), blood glucose levels rise.
Risk Factors
Risk factors for gestational diabetes include:
- Obesity
- Prior history of gestational diabetes
- Prior delivery of a high birth weight infant (over 9 pounds)
- Family history of type 2 diabetes
- History of polycystic ovary syndrome (PCOS)
- Ethnic background (African American, American Indian, Asian American, Hispanic, or Pacific Islander)
- Prediabetes
Warning Signs and Symptoms
Gestational diabetes typically does not cause noticeable signs or symptoms, which is why screening tests are crucial. Rarely, increased thirst or urinary frequency may be noticed.
Diagnosis
Gestational diabetes is diagnosed with blood tests, usually performed between the 24th and 28th weeks of pregnancy. The screening glucose tolerance test involves drinking a sugary beverage and having blood drawn to test glucose levels an hour later. Additional testing may be required if the screening test is abnormal.
An oral glucose challenge test (OGTT) may also be used, where blood glucose levels are measured at baseline and then 1, 2, and sometimes 3 hours after consuming a sugary drink. A blood glucose level of 140mg/dL or higher on this test identifies 80% of women with gestational diabetes. Lowering the cutoff to 130mg/dL increases the identification rate to 90%. Women with blood glucose greater than 130mg/dL are typically recommended to take another diabetes screening test that requires fasting.
Another test, called glycosylated hemoglobin or hemoglobin A1c, measures the average blood glucose level over the past few months.
Screening
All pregnant women should be screened for gestational diabetes, typically between the 24th and 28th weeks of pregnancy.
Treatment
Proper treatment for gestational diabetes is essential to reduce the risk of complications. Treatment includes maintaining a proper diet, focusing on nutritional modification. Regular exercise can also contribute to glucose control.
Monitoring blood glucose levels at home and testing urine for ketones may be recommended. If diet and exercise are insufficient, insulin therapy may be required.
Diet Plan
While there is no specific diet recommended for all women with gestational diabetes, following a meal plan can help control blood sugar levels and avoid complications. It is important to eat a variety of foods, opt for smaller portions throughout the day, limit consumption of foods high in simple sugars, and include high-fiber options.
Prognosis
Most women with gestational diabetes who receive proper treatment deliver healthy babies. However, if blood glucose levels are not well-controlled, the risk of complications increases. Some women may develop type 2 diabetes after pregnancy, but this risk can be reduced by following a good nutritional plan, exercising, and maintaining a healthy weight.
Complications for the Mother
- Cesarean birth
- Preeclampsia (high blood pressure and protein in urine)
- Risk of type 2 diabetes after pregnancy
Complications for the Baby
Gestational diabetes can cause the baby to be larger than normal and increase the risk of low blood glucose levels after birth. Other complications may include jaundice, respiratory distress syndrome, and an increased chance of death before or following birth. The baby is also at a greater risk of becoming overweight and developing type 2 diabetes later in life.
Prevention
While gestational diabetes cannot always be prevented, maintaining a healthy weight and following a good nutritional plan can decrease the chances of developing the condition. It can also reduce the risk of developing type 2 diabetes after pregnancy.
Subscribe to MedicineNet’s Diabetes Newsletter
By clicking "Submit," I agree to the MedicineNet Terms and Conditions and Privacy Policy. I also agree to receive emails from MedicineNet and understand that I may opt out at any time.